The real shadow pandemic of gender-based violence, underlying these mental health disorders, is ignored by health practitioners, researchers and policymakers
NEWS headlines alert us to surging rates of mental ill health in young people and women. People attribute it to the COVID pandemic, calling mental ill health the “shadow pandemic”.
The real shadow pandemic of gender-based violence, underlying these mental health disorders, is ignored by health practitioners, researchers and policymakers. Gender-based violence is seen as one of the social determinants of health and put in the “too hard” basket.
Gender-based violence, which includes domestic or sexual violence, is not addressed to any great extent in health systems, particularly mental health settings. In the MJA this week, my colleagues and I argue that transformation of health systems is urgent if we are to prevent the burden of disease from the chronic social condition of gender-based violence for women and children, particularly for Indigenous peoples.
The gender evidence is clear. The National Survey of Mental health and Wellbeing released this month finds that almost half of young women aged 16–24 years report experiencing a mental health disorder in the past year, compared to a third of young men. Young women are also most at risk of domestic and sexual violence in the community. Young women were also found to be most at risk of post-traumatic stress disorder, self-harm and eating disorders; all strongly associated with abuse and violence. Further, women of all ages were at higher risk than men for all mental disorders, except substance use disorder.
Some researchers feel this gender difference is due to hormonal influences. Others feel that gender-based violence underlies this increase in mental health issues and needs to be urgently addressed in health settings. Over half of the women in the National Survey sought help for their mental health, mostly seeing a GP (46%), a psychologist (25%), other mental health professional (10%) or a psychiatrist (8%). However, we know that general practice and the mental health system are ill equipped and poorly resourced to identify and respond to domestic and sexual violence.
We need a revolution in the health system to deliver trauma- and violence-informed care to meet the needs of victim/survivors of domestic and sexual violence. A basic start in this transformation is rather than practitioners asking “what is wrong with you?” and diagnosing a mental health disorder, practitioners ask “what has happened to you?”.
Systematic review evidence from voices of victim/survivors tell us we need to deliver a first line response across the health system that provides the CARE model (Figure 1).
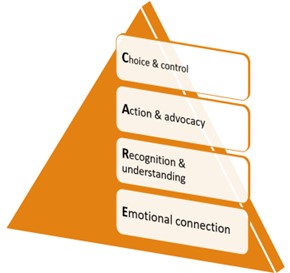
Currently, the health system is not providing this basic aspect of response in health settings to gender-based violence.
Further, the guiding principles of trauma- and violence-informed care need to be enacted. These include safety (physical, emotional, spiritual and cultural), trustworthiness, transparency, collaboration and respect for diversity. This last aspect is essential for Indigenous women, who experience overt racism and discrimination in health settings. Strategies could include:
- Establish self-care and safety plans for staff and clients;
- Be aware of and communicate about trauma triggers and safety needs;
- Use a person-centred approach, shared decision making and goal setting, in context of an understanding that trauma can impact cognitive functioning;
- Work to prevent biases based on gender, race, age, ethnicity, sexual orientation, ability or geography;
- Promote healing value of traditional cultural connections;
- Recognise and respond appropriately to historical and intergenerational traumas.
In addition, the health system needs to employ lived experience workers in the system, using strengths-based and skill building approaches. This is starting to take off in the mental health system and showing some benefits to self-reported recovery and empowerment. But without the focus on survivors of abuse and violence, the underlying traumas that women experience are hidden. For Indigenous women, a trusting relationship with the person talking is critical, including holding the space and incorporating cultural methods of communication gently and indirectly to understand the effects of trauma.
Health care policy needs to invest in a system response to gender-based violence if we are going to ameliorate the mental and physical health burden in Australia. Health professionals require training, including cultural safety and antiracist practice, scripts, referral pathways; and leadership support (Figure 2).
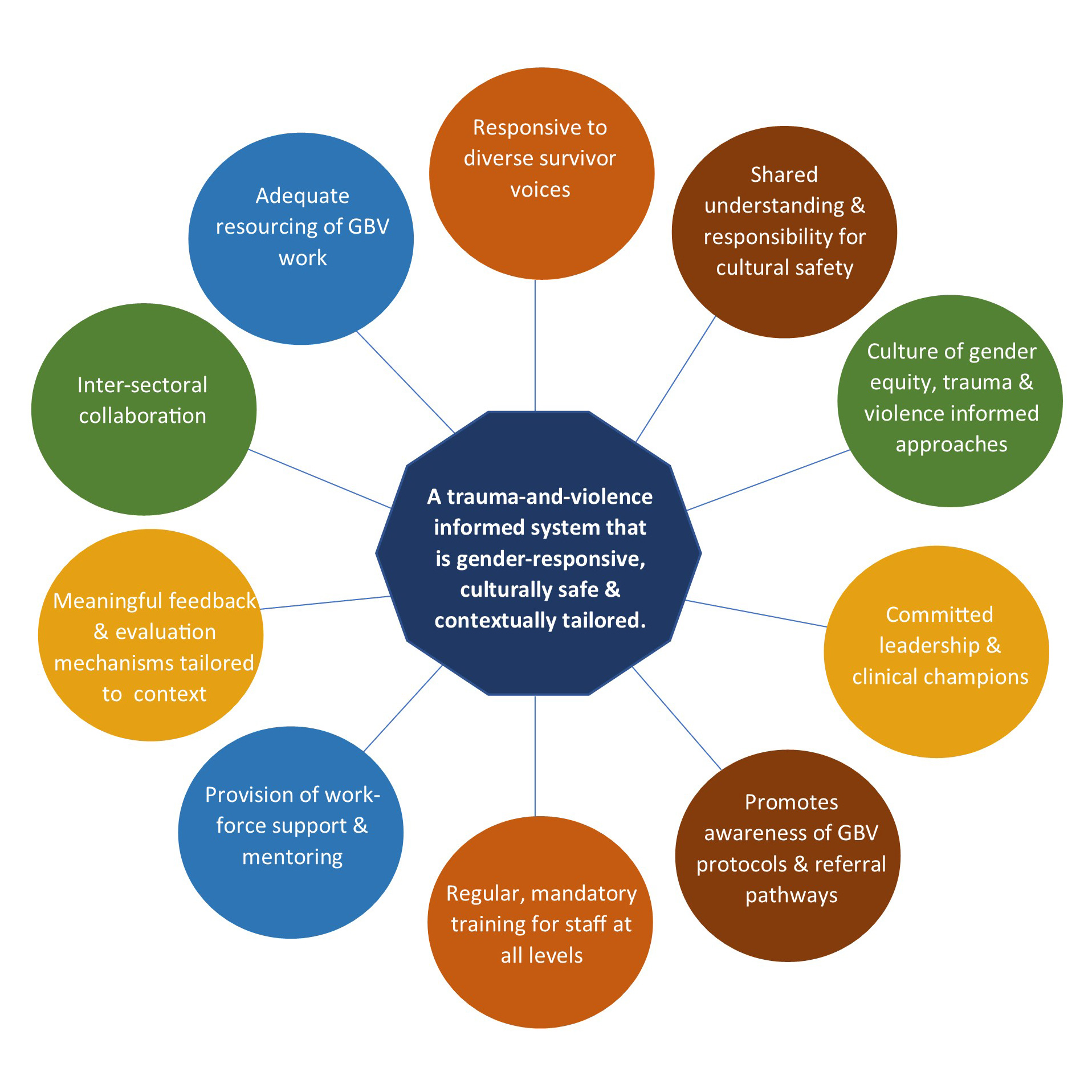
Safer Families Centre is working with a lived experience group, called the WEAVERS, to codesign models of care and this is key to reforming the health system. As one of the WEAVER survivor advocates, Fiona recently said when she was copresenting with me:
I have found trauma-informed services to be quite rare, which can make sourcing services really difficult. In trauma-informed services you are listened to and validated, you don’t have to fight to be believed. You don’t need to keep telling your story, which in itself is very triggering, you can just be. For example, going to an art therapist is wonderful; I have found that I can release trauma through art with little to no triggering. It is the perfect thing as it is not verbal
Professor Kelsey Hegarty is an academic GP who holds the joint Chair in Family Violence Prevention at the University of Melbourne and the Royal Women’s Hospital. She leads the NHMRC Safer Families Centre of Research Excellence (see saferfamilies.org.au) and co chairs the Melbourne Research Alliance to End Violence against Women (MAEVe).
The statements or opinions expressed in this article reflect the views of the authors and do not necessarily represent the official policy of the AMA, the MJA or InSight+ unless so stated.
Subscribe to the free InSight+ weekly newsletter here. It is available to all readers, not just registered medical practitioners.
If you would like to submit an article for consideration, send a Word version to mjainsight-editor@ampco.com.au.

 more_vert
more_vert
“The gender evidence is clear. The National Survey of Mental health and Wellbeing released this month finds that almost half of young women aged 16–24 years report experiencing a mental health disorder in the past year, compared to a third of young men.”
Evidence? This is a self reported survey. Open to so much bias. Firstly – There were 5,554 fully responding households in the study, a response rate of 57.1%.” Are Australian males known for volunteering poor mental health??
From the article
“However, we know that general practice and the mental health system are ill equipped and poorly resourced to identify and respond to domestic and sexual violence.”
I was wondering why Australian GP’s are so poorly equiped? There seems to be training in this through the GP registrar training programs. Plenty of post graduate training, webinars, workshops etc.
And how does GP care in Australia compare to other first world nations?
The majority of domestic violence victims are female but certainly the majority of violence victims overall are male and the majority of perpetrators are male ….which means that this is a male problem.
Please see our study from the 2007 dataset which found strong associations between exposure to a Gender Based Violence and mental disorders (including depression and PTSD) and attempted suicide amongst women. Our paper was published in the Journal of the American Medical Association (JAMA) https://pubmed.ncbi.nlm.nih.gov/21813429/
yes there is a domestic violence problem.
but the stats keep showing that the majority of overall violence victims ( not just domestic ) and murder victims are males.
violence is not just a female problem despite the media’s attempt to make it so
‘The gender evidence is clear. The National Survey of Mental health and Wellbeing released this month finds that almost half of young women aged 16–24 years report experiencing a mental health disorder in the past year, compared to a third of young men. Young women are also most at risk of domestic and sexual violence in the community.’
A juxtaposition of two sentences designed to conflate, where there is no necessary causal relationship: which is not to diminish the issue of domestic violence, but whatever the amount of that violence, it is not the exclusive cause of poor mental health.