PLANNING to support the recovery of patients who experience severe complications of coronavirus disease 2019 (COVID-19) is critical, say rehabilitation experts, with one saying “we don’t know what survivorship looks like”.
“We now need to prepare for the recovery phase because surviving may not be the same as living,” the authors wrote in an MJA Perspective that outlined the rehabilitation plan developed by the NSW Rehabilitation Community of Practice.
The authors acknowledged that Australia had managed the COVID-19 crisis well so far, noting that planning had been key to this success, and said that focus was now needed on a rehabilitation response strategy.
Speaking to InSight+, Associate Professor Steven Faux, Director of the Rehabilitation Unit at Sydney’s St Vincent’s Public Hospital and lead author of the MJA article, said just 1–2% of patients with COVID-19 developed severe disease. In Australia, more than 150 patients have been admitted to intensive care units (ICUs) with COVID-19.
Associate Professor Faux said patients who had been ventilated for more than 7 days could develop swallowing and breathing difficulties, and one in three patients would develop critical care neuropathy or critical care myopathy.
“At least half of COVID-19 patients who have been ventilated for more than a week will have difficulty walking and some will take up 150 days to be able to walk independently,” he said.
Professor Andrew Udy, Professor of Critical Care Research at Monash University, and Deputy Director (Research) at The Alfred ICU, said ICUs strove to limit the impact of ventilation on the lungs, but there were additional complexities in managing patients with COVID-19.
“What we do routinely is use a ventilation strategy that is non-injurious, trying to limit the pressure, limit the volume, limit the amount of work that the ventilator is doing – doing just enough to support the patient while not injuring the lungs,” Professor Udy said.
“When people develop severe pneumonitis – as is the case with COVID-19 – the lungs become soggy and stiff, and difficult to ventilate. We may need to use higher and higher pressures and that’s where we get uncomfortable and [consider] that the ventilator may be harmful and we need to try another strategy.”
And while there were still many unanswered questions around the pathophysiology of COVID-19, Professor Udy said there was clearly also an insult to the lungs from the virus itself.
“In patients who get very sick, that involves inflammation, microthrombosis, and that in turn results in impaired gas exchange,” he said. “That’s why patients with severe COVID-19 are often very hypoxic.”
The MJA authors noted that patients who developed stroke or cardiac complications of COVID-19 would require rehabilitation for up to 6 weeks, with some requiring lifelong support.
Associate Professor Dion Stub, interventional cardiologist at Alfred Health, said 15–30% of patients admitted to hospital with COVID-19 would have some cardiac involvement. He noted, however, that Australia had been fortunate so far in largely avoiding such complications.
“Cardiac complications can range from mild cardiac inflammation with troponin leak to full-blown thromboembolic complications, so that’s acute myocardial infarction, stroke, or pulmonary embolism,” he said, adding that acute viral infiltration of the heart or blood vessels with acute myocarditis or endothelialitis leading to vasculitis was also possible.
“What’s unknown is whether COVID-19 will have any long term sequelae on cardiac function.”
Associate Professor Stub agreed that greater focus on the potential needs for rehabilitation was needed.
“We have been very focused on gearing up our acute services, and there needs to be some attention made to gearing up subacute and rehabilitation facilities.”
Associate Professor Faux said a multidisciplinary approach to rehabilitation after severe COVID-19 was essential. In addition to support from rehabilitation physicians and physiotherapists, patients also may need access to speech pathology, dietetics and occupational therapy.
Psychologists were also often required, with some patients developing depression, anxiety, and post-traumatic stress disorder, he said.
Dr Faux said a “game plan” had been needed to tackle the complexities of post-acute care of patients with COVID-19, so a Community of Practice was established to advise the NSW Ministry of Health.
The subsequent development of the staged COVID-19 escalation plan dealt with crucial issues such as de-isolation protocols and innovative models of care, including the use of mobile rehabilitation teams, he said.
By providing rehabilitation and discharge planning services in acute hospitals, Associate Professor Faux said these mobile teams had resulted in discharging almost half of their patients directly home, avoiding inpatient rehabilitation admissions.
“Those teams are now starting to treat COVID-19 patients, but they weren’t well utilised initially.”
Tele-rehabilitation services could also play a key role in aiding patients’ recovery, he said.
“We have been using telerehabilitation for some years in this country because of our rural population, so we are very well set up to provide this support.”
Professor Udy, who also co-leads the SPRINT-SARI Australia Surveillance Study on patients with COVID-19 in Australian ICUs, said planning for patient recovery should start in the ICU.
“It’s critical that we start thinking as early as possible about promoting functional recovery,” he said.
“We need to promote early physical rehabilitation, even in the ICU and acute wards, mobilising people and getting people out of bed, even when they are on a ventilator. We need more research on that.”
And more research was also needed on organ function recovery, Professor Udy said.
“We need to understand the long term health care consequences of COVID-19. There may be long term impacts on lung function, cardiac function, immune function, haematological function … there may be changes in a patient’s immunophenotype that could be long-lasting.
“It’s a very new disease,” he said. “We don’t know what survivorship looks like.”

 more_vert
more_vert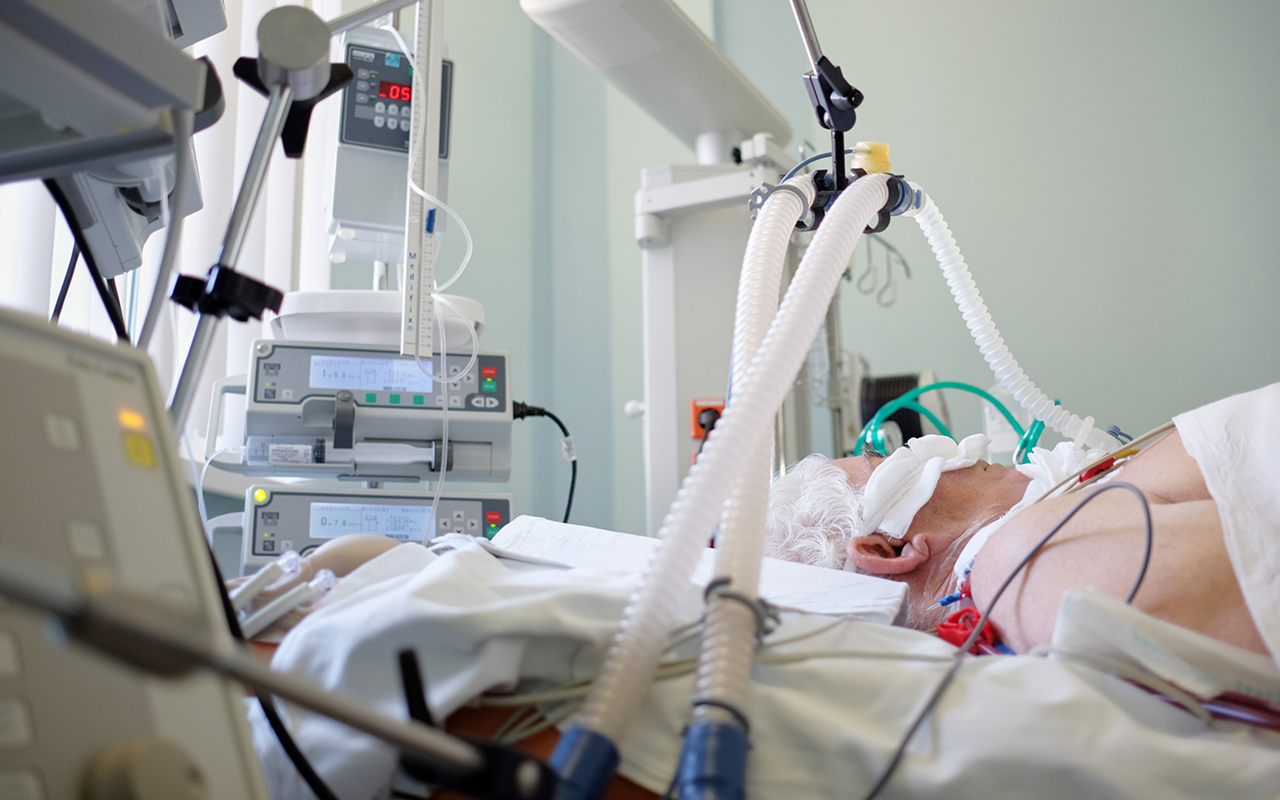
It’s absurd that there are people in this forum actively advocating ‘killing off’ nursing home residents with COVID, intentionally. For what reason? Free up care homes? Whilst it is inevitable that a proportion of our elderly contract influenza or other respiratory diseases each year and dies as a result, that is a completely different argument compared with wilfully passing a highly lethal disease into nursing homes or wilfully letting helpless institutionalised residents catch the disease. Would the same author suggest passing COVID-19 into supported homes, prisons, mental health facilities, asylum seeker centres?! Have you asked for consent from the affected parties?
Straight out of WWII such individuals would be labelled as Nazi sympathisers and be shunned in society. I hope the same still apply today.
too risky to allow people across borders with no known Covid -19 scren