WHEN actor Will Smith smacked comedian Chris Rock at the Oscars two weeks ago, it inspired a torrent of water cooler discussion.
For weeks, people debated all aspects of the incident: the violence on a world stage, whether Will Smith needed to defend his wife Jada Pinkett Smith when she has her own voice, whether comedians should use a person’s medical condition as fodder for laughter.
Rock was making fun of Pinkett Smith, saying “Jada, can’t wait for GI Jane 2,” when she arrived at the ceremony with a bald head. However, she wasn’t just starting a new fashion trend; Pinkett Smith has alopecia areata, an autoimmune condition that leads to hair loss.
“Once in a career” treatment game changer
Although he calls the Will Smith incident a “circus performance”, world leader in the treatment of hair loss, Professor Rodney Sinclair, Professor of Dermatology at the University of Melbourne and Director of Epworth Dermatology, said there have been some benefits from the drama. For one, it has alerted people to the distress of having alopecia areata.
Second, it highlights the dramatic treatment changes that have recently been developed.
Until a few years ago, there wasn’t much that could be done for alopecia areata.
“When patients walked in the door, even 10 years ago, they’d say ‘what’s caused it’. We’d just shrug our shoulders. And they’d say, ‘How are we going to treat it?’ We’d say, ‘we’ve got no idea’. And they’d say, ‘what’s going to happen in the future?’ We’d say, ‘we don’t really know, we have to just wait and see’,” Professor Sinclair, told InSight+.
Not so anymore. In fact, the entire landscape for alopecia areata has changed in a very short period. Two weeks ago, an article in the New England Journal of Medicine showed exactly how far treatment has come.
“This is a once in a career game changer. It’s a little bit like when roaccutane came out for acne or when biologics first became available for rheumatoid arthritis. This totally changes the trajectory of the lives of people affected by alopecia areata,” Professor Sinclair explained.
The trial, on which Professor Sinclair was a co-author, showed for the first time that you could achieve high response rates in people with severe alopecia areata with a Janus kinase (JAK) inhibitor called baricitinib. Janus kinases are enzymes associated with cytokine receptors on the surface of cells, and are involved in inflammatory and immune responses.
“The trial participants all had chronic alopecia areata disease, with disease duration of at least 6 months, or more commonly more than 12 months. They all had somewhere between 50% and 100% hair loss, with severity skewed towards the severe end.
“The endpoint of the trial was to have minimal disease. So, it’s not 100% remission, but if they can get their level of scalp affected to less than 20%, then that is a meaningful improvement and their residual disease load can be simply managed by intralesional injection of corticosteroid or topical therapy, or can be easily concealed. That endpoint was achieved in 17% of patients with the 2 mg dose and in 33% with the 4 mg dose of baricitinib,” Professor Sinclair explained.
Alopecia areata “not caused by stress”
During the past decade, research has also clarified the causes of alopecia areata. It’s a complex polygenic disease, with 17 gene variants already identified that increase an individual’s susceptibility to alopecia areata, although most people only have four or five of those gene variants. The number and combination of these variants determine the threshold for an environmental trigger that will initiate a patch of hair loss in a susceptible individual.
“That environmental trigger is almost certainly intercurrent viral infection that activates the immune system, and increases circulating levels of interferon-γ gamma. And it’s almost certainly nothing to do with stress,” Professor Sinclair explained.
Most people are under the misconception that stress causes alopecia areata, which is something Professor Sinclair wants to correct.
“When you allege that the hair loss is caused by stress, the implication is that the patient has brought this on themselves by their inability to manage their circumstances. And I think not only is that factually incorrect, it’s damaging,” he told InSight+.
“The effect of interferon-γ is that it leads to collapse of hair follicle immune privilege, which means that the hair follicles are now susceptible to autoimmune attack.
“The autoimmune attack leads to hair fibre breakage radiating outwards from that initial individual fibre, producing circular patches of hair loss.”
When a person has one patch of hair loss, it lowers their threshold for developing a second patch. If there is another environmental trigger while the person has a second patch, they will develop another patch and so on.
Disease self-accentuation is why it’s important that people receive the right treatment when they develop their first patch.
Impact of alopecia areata is significant
Alopecia areata is the most common auto immune disorder in Australia, and its burden is profound. Unfortunately, patients often suffer in silence.
“Because historically there was no effective treatment, people haven’t endeavoured to quantify the patient distress associated with alopecia areata,” Professor Sinclair said.
“Patients were basically just sent away. When you talk to the patient support groups, they say the all too common experience among affected members was a disappointing medical encounter.”
For young people, it can be particularly damaging, especially for boys.
“Girls have long hair that they can tie back in a ponytail, and they can conceal up to 20–30% hair loss without having to disclose to anyone that they’ve got alopecia. Because of the fashion with boys’ hair, even one tiny patch is immediately obvious. And that often leads to teasing and bullying at school, school absenteeism, social withdrawal, depression and profound psychological morbidity,”
As Professor Sinclair has previously written in the MJA, most childhood suicides related to alopecia areata are in boys.
Treatment in general practice
For patients presenting with acute alopecia areata (disease duration < 6 months), Professor Sinclair said it can be managed either with intralesional triamcinolone, or topical ultrapotent corticosteroids such as diprosone OV.
“But if they’ve got any doubts or any concern about the diagnosis, because the diagnosis is not always straightforward, or if it’s chronic alopecia areata, then refer the patient,” he advised.
It’s also important to know that the old mantra of watchful waiting is not appropriate.
“The more disease you have, the worse your prognosis,” he said. “The longer duration of disease you’ve had, the worse your prognosis. The idea of watching to see whether it gets better by itself is poor medicine.”
More information about alopecia areata.

 more_vert
more_vert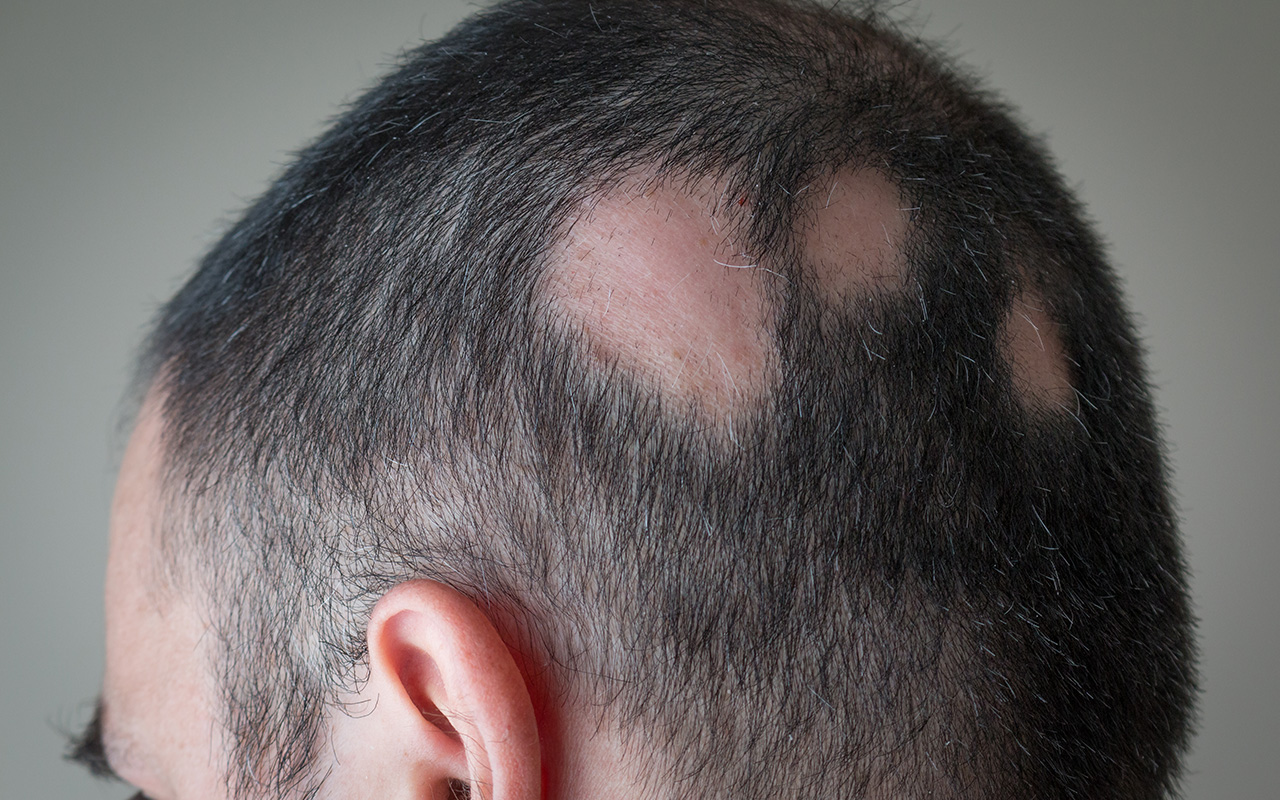
With the efforts of Prof. Sinclair in Ausralia as well as other clinicians around the world including Brett King in USA, two biological drugs Baricitinib, and lately Retlicitinib, have been approved for treatment of severe cases of alopecia areata. Remained questions are: who is considered to be severe case to be eligible for these drugs? As alopecia areata has vast psychosocial burdens, is extent of scalp hair loss represents the disease severity per se? The other remained question is cost-benefit of biological drugs. Researchers endeavour continues in order to determine eligible patients for these drugs and convince PBS to subsiduze these drugs according to their efficacy, safety and cost-benefit.
Fantastic article. I was an unfortunate statistic of AU in 2021, lost all my hair very quick after a viral infection. JAK have kept me off anit-depressants and probably saved my livelyhood. I am so happy research continues and medication becomes avaliable and affordable over the years.
We are currently paying $436 for 3 months ( 180 tabs , 2 per day) supply of Tofacitnib compounded medication in Sydney. The results in 4 months for my teenage son, who has suffered for 3 years, has been life changing. Thank you to all the researchers, Dr Sinclair and all dermatologists who have supported us in getting to this point. Much appreciated.
Thank you Dr Sinclair for your clinical work and advocacy on our behalf.
I have alopecia universalis and have been told of this treatment by my Dermatologist but the current cost is out of my reach, so I wait with eagerness for it to be put on the PBS.
excellent News, But it will be years before this treatment reaches Rural Australia.
These medications are expensive. Before the PBS subsidize a medication, the efficacy and safety data will need to be evaluated by the TGA,. Once approved by the TGA, the PBAC will need to consider the cost benefit analysis of treating alopecia areata with this medication. If the PBAC make a positive recommendation, then the cabinet of the Federal Government will need to approve the medication before it is listed on the PBS. This very detailed analysis protects the Australian tax payers and ensures a finite resource (our taxes) are directed towards the greatest community benefit.
Unfortunately the process delays patients in need accessing these potentially game changing medication. https://onlinelibrary.wiley.com/doi/10.1111/bjd.20712
The challenge for the the pharmaceutical industry, PBAC and for us as researchers is to put a dollar value on the impact of hair loss and on the benefit of treatment. Work on this is continuing.
Sadly, at the moment these medications are not included in the PBS in Australia and retail for approximately $1300 for 90 tablets with patients having to take 2 per day. Until this class of medication become included on the PBS for alopecia, sufferers will be no closer to a treatment as I doubt there are many people who can afford this medication.
Thankyou for this priceless work.
I’m looking forward to the breakthrough in the UK and the world to help with this disease.
My mum had total.i have total and my sister has patches.m8ne has been approx 6 months