SUICIDE is a major public health concern worldwide. Yet suicide has only emerged in the past half century for Aboriginal and Torres Strait Islander (hereafter, respectfully referred to as Aboriginal) peoples. Since then, the increase in suicide deaths in Aboriginal communities has been alarming, with an increase of 49% between 2006 and 2018. Suicide rates in Aboriginal peoples are at least twice the rate of non-Indigenous people across gender and age groups; for youths aged 15–24 years, the rate is over five times higher.
COVID-19 does not discriminate against age, race, religion or socio-economic status. Still, the impact of the COVID-19 pandemic is disproportionately greater for Aboriginal peoples and communities, due to the systemic historical, political, social and economic determinants of health that influence the uptake, access and efficacy of health and mental health services. These systemic factors underscore the Social and Emotional Wellbeing (SEWB) model. This model is a strengths-based, holistic health framework for Aboriginal peoples, which reflects the complex interrelationships between self, protective cultural domains, and the encompassing determinants.
The SEWB model represents a decolonising strategy to promote wellbeing. It features dominantly in the National Strategic Framework for Aboriginal and Torres Strait Islander Peoples’ Mental Health and Social and Emotional Wellbeing, which was endorsed by the Australian Health Ministers’ Advisory Council and Aboriginal communities across Australia.
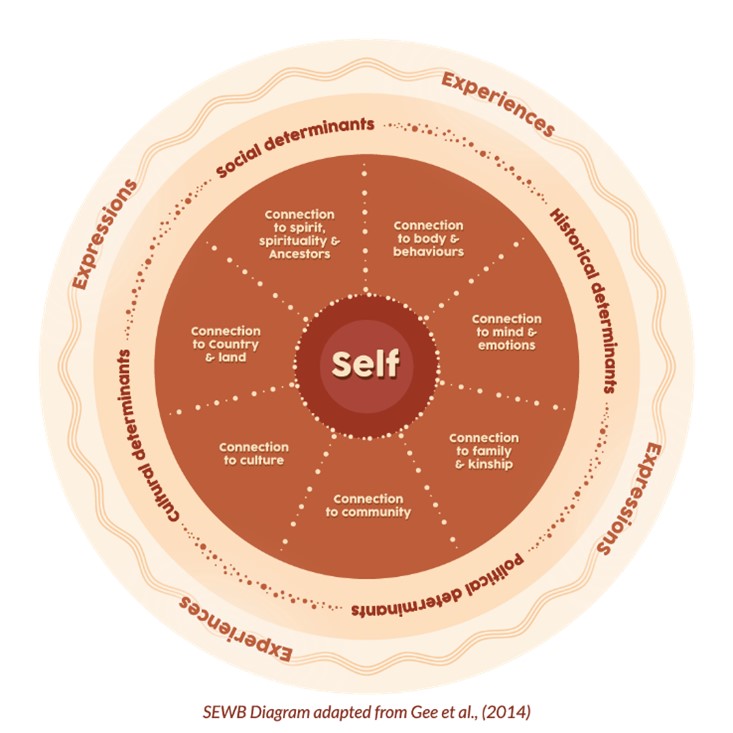
Figure 1. Social and Emotional Wellbeing (SEWB) model
The SEWB model consists of seven cultural, interrelated, and overlapping domains of Aboriginal selfhood: connection to spirit/Ancestors, body/behaviour, mind/emotions, family/kinship, community, culture, and Country/land. Programs designed to strengthen social and emotional wellbeing and build individual, family and community resilience in Aboriginal communities have been successful across various sites across Australia. For example, cultural wellbeing and SEWB programs have been developed under the National Empowerment Project (NEP). The NEP was established in 2012, and is an Aboriginal-led research collaboration, which involved extensive multisite community consultations and codesigned programs, including the Cultural, Social and Emotional Wellbeing (CSEWB) program.
Participants of the CSEWB programs experienced reduced psychological distress and reported long term benefits, including improved relationships within families and communities, strengthened social support network, self-confidence and resilience, which directly, indirectly and interactively contribute to improved cultural identity and social and emotional wellbeing. This may be because in addressing the protective factors of social and emotional wellbeing, other risk factors such as physical and mental health, education, employment, housing, and family and community relationships may improve given the interrelated nature of these factors. Cultural, social, and emotional wellbeing is a protective factor against suicide risk for Aboriginal peoples.
Similarly, other suicide prevention strategies for Aboriginal peoples must address the SEWB domains to be effective. For example, strategies must reflect the connection to culture and community by ensuring that programs and services are culturally safe and responsive. Hence, it is crucial to engage communities and encourage community ownership and governance from the beginning. Local communities have proprietary knowledge of their cultural beliefs and practices, which are diverse and differ across groups and locations. Moreover, local communities possess the insights to better identify needs and priorities within their communities and respond to them in a culturally safe and responsive way, significantly enhancing the uptake and effectiveness of such efforts.
It is no coincidence then that the criteria for best practice programs and services recommended by the Centre of Best Practice in Aboriginal and Torres Strait Islander Suicide Prevention (CBPATSISP) are Indigenous ownership, community leadership, consultation and codesign, continuous evaluation, cultural responsiveness, and capacity building. These criteria embrace a strengths-based and self-determination approach (here and here) by empowering Aboriginal communities to have control over their human right to health and wellbeing, while reflecting the strengths of local communities. In addition, CBPATSISP focuses on diverse groups, and privileges the voices of Aboriginal peoples with lived experience of suicide. For example, evidence suggests that the factors influencing social and emotional wellbeing may be lifespan specific; therefore, efforts that target youth suicide risks would benefit from being informed by youths’ perspectives of what works to strengthen their social and emotional wellbeing.
The CBPATSISP was established to address the impact of suicide, loss and grief on Aboriginal communities by promoting the development and implementation of culturally safe and responsive, and evidence-based suicide prevention programs and services. These best practices are informed by the research findings of the Aboriginal and Torres Strait Islander Suicide Prevention Evaluation Project (ATSISPEP) which is a government funded initiative to address Aboriginal suicide. The objectives of the ATSISPEP were to evaluate Aboriginal suicide prevention programs and services, to identify community needs with the aim of developing a culturally safe and responsive suicide prevention programs and services evaluation framework. Suicide risks and mental health issues in Aboriginal peoples have been thrown into the spotlight amid the COVID-19 pandemic, highlighting the increasing relevance of the efforts of the ATSISPEP and CBPATSISP.
While culture is listed as one of the domains under the SEWB model, culture is infused throughout the model of holistic health and is central to the mental health and wellbeing of Aboriginal peoples. Cultural practice, beliefs and values passed down through generations are intrinsically and inexorably linked, if not foundational, to the strong connections to Country, spirit, body, mind and emotions, family and kinship, community and Country. Culture shapes one’s worldview and dictates what is sacred and important to Aboriginal peoples, as reflected in their strong connection to the land they live on. Importantly, culture guides Aboriginal peoples’ decision to access health services and determines their acceptance and adherence to treatment. Access and acceptance will determine the effectiveness of suicide prevention strategies.
On the other hand, cultural safety and responsiveness on the part of clinicians will help or hinder the delivery of health services to Aboriginal peoples. For Aboriginal peoples, wellbeing and the ability to overcome the emotional distress and adverse mental health effects of COVID-19 is dependent on the interaction between culture and other determinants, including individual psychosocial factors.
A strong connection to family, kinship and the community underscores the social and emotional wellbeing of Aboriginal peoples; subsequently, increased experiences of racism in addition to strict social isolation rules imposed in Australia in response to the COVID-19 pandemic inevitably cause anxiety, fear and emotional distress. Together with a sense of disempowerment and loss of control, these emotional states may lead to an increase in dysfunctional coping strategies and behaviour, including alcohol and drug use. The bidirectional and interactive relationships between these risk factors may then trigger a downward spiral in social and emotional wellbeing, thereby increasing suicide risk. In the midst of, or after, the COVID-19 pandemic, re-establishing and rebuilding the connections that strengthen the social and emotional wellbeing of Aboriginal peoples have become increasingly important.
Suicide prevention is a complex issue globally and there is little evidence to guide prevention strategies. Even less research is being done on culturally safe and responsive strategies. Furthermore, there is a lack of timely data on the evaluation of the effectiveness of existing suicide prevention strategies, policies and implementation. Further research is warranted. Suicide prevention efforts that encompasses the SEWB model and puts “Aboriginal health in Aboriginal hands” may be a promising starting point.
Professor Pat Dudgeon is Director of the Centre of Best Practice in Aboriginal and Torres Strait Islander Suicide Prevention and Chief Investigator of Transforming Indigenous Mental Health and Wellbeing project. She can be found on Twitter at @cbpatsisp.
Dr Ee Pin Chang is Research Associate in the School of Indigenous Studies at the University of Western Australia. She is passionate about justice, equity, health, and wellbeing in disadvantaged. She can be found on Twitter at @EePinChang1.
Dr Kate Derry is Research Associate in the School of Indigenous Studies at the University of Western Australia. She uses evidence-based approaches and strengths-focused solutions to empower Indigenous peoples. She can be found on Twitter at @KateLorenDerry.
The statements or opinions expressed in this article reflect the views of the authors and do not represent the official policy of the AMA, the MJA or InSight+ unless so stated.

 more_vert
more_vert