CARING for patients at their most vulnerable has a way of cutting through life’s worries. However, I was unprepared for my own vulnerability when I was diagnosed with grade 3 triple negative breast cancer at the age of 47 years. Being a patient with cancer is the hardest challenge I have ever faced.
Rolling over in bed at 3am, my hand landing on a hard lump in my breast instantly woke me with a feeling of dread that changed my life forever. I lay there until morning trying to tell myself it was just a cyst, but my medical training told me otherwise. Years of treating breast lumps, reassuring the worried and arranging urgent scans and biopsies prevented me from being falsely reassured. Suddenly, it was me with the breast lump and the crazy cancer journey began. At first light, I woke my husband and we made a plan. First, we had to get our daughter to hospital for day surgery for complications after a dislocated elbow. Next, I rang my GP and made an urgent appointment.
Reassuring my daughter and admitting her to hospital provided distraction but only intensified my feeling of disbelief. My husband, also a doctor, and I kept exchanging glances filled with silent meaning. Suddenly, all the years of emergencies and breaking unexpected news faded into the background as I faced my own mortality. As doctors we are trained to save the lives of others. We still have a long way to go to deal with all the challenges that come with saving our own. The transition from doctor to patient is a huge task, and when it happens overnight, it blindsides you in a way that takes extraordinary strength and determination to manage.
Discovering the breast lump was followed by more investigations and specialist appointments than I had ever experienced. Treatment options are overwhelming at a time when even the possibility of cancer seems incredulous. I had no family history of breast cancer and no modifiable risk factors. Breast cancer was something that I can honestly say had never crossed my mind. I enjoyed work, had great family and friends and was fit and healthy, running 5–10 km several times a week. Knocked sideways does not begin to do justice to how I felt.
My GP arranged an urgent breast ultrasound and mammogram. The mammogram happened quickly, with me confidently trying to tell myself there would be nothing to find. The ultrasound, however, brought down my thinly veiled bravery. Looking at the ultrasound as the sonographer scanned over the lump it was obvious it was something to be concerned about. My concern was only heightened when a lengthy examination of my axilla found further abnormalities. The radiologist came in and recommended a core biopsy of the breast lump and a fine needle aspirate of axillary lymph nodes.
I held it together while we arranged for biopsies the following morning, but I fell apart as I walked down the corridor of the hospital desperate to avoid seeing anyone I knew. Tears flowed freely. As I drove home, I openly wept. Medical knowledge is a privilege, but it does not allow you the time to believe things may be okay and takes away the opportunity for someone to break the news to you gently.
While I was having the investigations, my husband was able to explain to our teenage daughter what was happening. Words were not necessary as I walked through the door sobbing. I was embraced by my family and comforted before we sat down and tried to get our thoughts around what was happening. We escaped for the weekend to enjoy a beautiful family bushwalk. With every step, I marveled at how I could be so fit and well and yet have cancer that had already spread to my lymph nodes. Knowing things medically and experiencing things personally are two vastly different perspectives.
The biopsies confirmed grade 3 invasive breast carcinoma with spread to the axillary lymph nodes. I was unprepared for the week that followed, with further staging investigations and visits to a breast surgeon and an oncologist. I went to work in a daze and told them I would be needing some time off. By the end of that week, I was booked to begin chemotherapy.
The tests further revealed triple negative breast cancer with a very high Ki-67 (proliferation index > 80%). Suddenly, it was not just about dealing with breast cancer but desperately hoping it had not spread beyond my lymph nodes. Survival statistics of metastatic triple negative disease made for terrifying reading.
The moment I learnt there was no distant spread was a moment of sheer relief and joy. It was so strange to feel thankful for only local spread to lymph nodes, yet this is the perspective that life-threatening cancer brings.
I was due to start chemotherapy in 2 weeks, but this would be a few days before Christmas. I made the first of many active choices that felt right for me and gave me a sense of some control. I asked if we could wait a week. I needed time to process and prepare.
It was a great decision. I spent a superb Christmas with my family, feeling well. We ate, laughed and cried; our lives forever changed.
It is safe to say we were unprepared for the immediate onslaught of dose-dense doxorubicin and cyclophosphamide chemotherapy, but at least I felt ready to start rather than feeling stunned and scared. I feel this made an enormous difference to my perspective and how I managed with all the chemotherapy side effects.
I approached chemotherapy as I imagine many high performing, task-oriented doctors would. I learnt how to manage all the side effects and did everything I could to survive. I meditated daily and during chemotherapy. I managed 16 cycles of chemotherapy without a port and no major complications. I walked in nature every day except for the 72 hours after the chemotherapy infusions, when I needed rest and ice packs to hands and feet to minimise the risk of hand-foot syndrome. I even managed a run after the first few doses knowing the benefits of vigorous exercise. My hair fell out after the second round and I embraced my bald head.
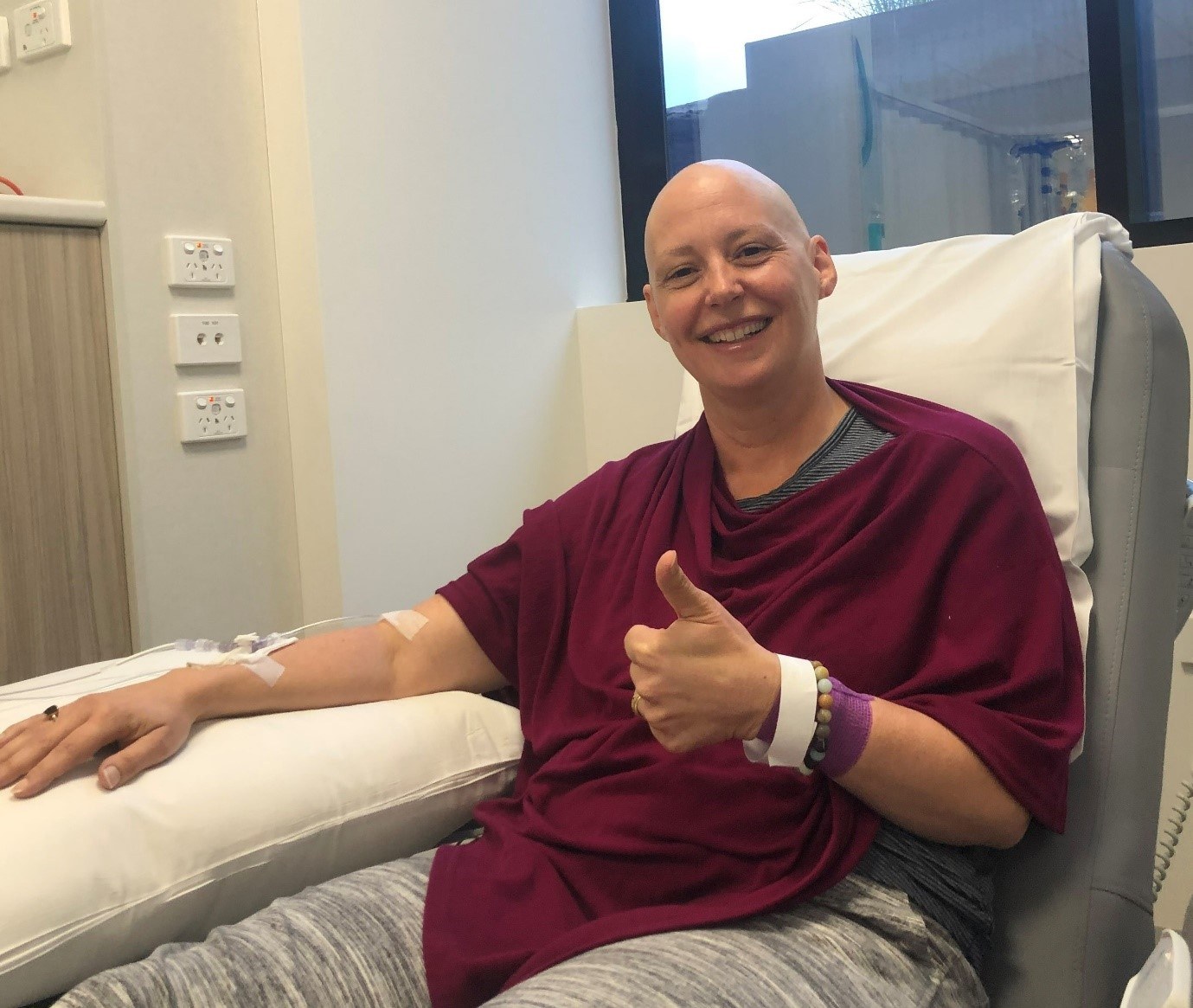
The twelve doses of paclitaxsol were better tolerated than the doxorubicin and cyclophosphamide, but each week came around so fast with no time to recover in between. Deconditioning despite daily exercise occurred rapidly. Combined with instant chemotherapy-induced menopause, mouth ulcers, constipation from antiemetics, sensitive skin, poor sleep from dexamethasone, and intense fatigue, it was a lot to manage. Just as I got some grey hair growth back on my scalp, I had lost all my body hair and my eyebrows and eyelashes fell out.
I had seen many patients through this journey. My medical knowledge and experience did not prepare me. I now know what they were not telling me. I had so much to learn! I also realise symptoms fade into the background when you are trying to survive.
After 5 months of chemotherapy, I tried to get some fitness back before surgery. The assistance of an exercise physiologist and cancer rehabilitation physiotherapist were invaluable, and I would like to see all cancer patients able to access them.
I was fortunate to have an amazing team and 5 months of chemotherapy to decide what treatment I wanted and plan for it. A month after finishing chemotherapy, I had a mastectomy, complete axillary lymph node dissection, and immediate autologous DIEP (deep inferior epigastric perforators) breast reconstruction.
Immediate autologous reconstruction meant I woke from the operation still feeling like I had a breast. Immediate breast reconstruction rates are low in Australia and more women requiring mastectomy for breast cancer should have access to this as an option. Access to the decision-making tool for breast reconstruction, BRECONDA, was valuable.
When you are busy saving your life, it is easy to believe losing a breast does not matter. However, the daily reminder of mastectomy can have more of an effect than just physical scars. Recovery has been slow and ongoing complications are part of my life now, yet the moment I learnt I achieved pathological complete remission was bliss. It was the miraculous news we had given our all to achieve.
As I return to work, I wish to use my experience to help others. The perspective of the patient journey I have gained will forever change me as a doctor. Being a patient has taught me so much more than my medical training could prepare me for. Strength, hope, determination, patience, courage and humour have been required. Understanding the fear, shame, guilt and embarrassment that accompanies the experience of doctors who become cancer patients is also important.
This patient perspective, through the lens of a doctor as the patient, will hopefully provide insights and reflection for all health professionals.
Dr Emma Warnecke is an Associate Professor in the Tasmanian School of Medicine at the University of Tasmania.

The statements or opinions expressed in this article reflect the views of the authors and do not represent the official policy of the AMA, the MJA or InSight+ unless so stated.
Rolling over in bed at 3am, my hand landing on a hard lump in my breast instantly woke me with a feeling of dread that changed my life forever. I lay there until morning trying to tell myself it was just a cyst, but my medical training told me otherwise. Years of treating breast lumps, reassuring the worried and arranging urgent scans and biopsies prevented me from being falsely reassured. Suddenly, it was me with the breast lump and the crazy cancer journey began. At first light, I woke my husband and we made a plan. First, we had to get our daughter to hospital for day surgery for complications after a dislocated elbow. Next, I rang my GP and made an urgent appointment.
Reassuring my daughter and admitting her to hospital provided distraction but only intensified my feeling of disbelief. My husband, also a doctor, and I kept exchanging glances filled with silent meaning. Suddenly, all the years of emergencies and breaking unexpected news faded into the background as I faced my own mortality. As doctors we are trained to save the lives of others. We still have a long way to go to deal with all the challenges that come with saving our own. The transition from doctor to patient is a huge task, and when it happens overnight, it blindsides you in a way that takes extraordinary strength and determination to manage.
Discovering the breast lump was followed by more investigations and specialist appointments than I had ever experienced. Treatment options are overwhelming at a time when even the possibility of cancer seems incredulous. I had no family history of breast cancer and no modifiable risk factors. Breast cancer was something that I can honestly say had never crossed my mind. I enjoyed work, had great family and friends and was fit and healthy, running 5–10 km several times a week. Knocked sideways does not begin to do justice to how I felt.
My GP arranged an urgent breast ultrasound and mammogram. The mammogram happened quickly, with me confidently trying to tell myself there would be nothing to find. The ultrasound, however, brought down my thinly veiled bravery. Looking at the ultrasound as the sonographer scanned over the lump it was obvious it was something to be concerned about. My concern was only heightened when a lengthy examination of my axilla found further abnormalities. The radiologist came in and recommended a core biopsy of the breast lump and a fine needle aspirate of axillary lymph nodes.
I held it together while we arranged for biopsies the following morning, but I fell apart as I walked down the corridor of the hospital desperate to avoid seeing anyone I knew. Tears flowed freely. As I drove home, I openly wept. Medical knowledge is a privilege, but it does not allow you the time to believe things may be okay and takes away the opportunity for someone to break the news to you gently.
While I was having the investigations, my husband was able to explain to our teenage daughter what was happening. Words were not necessary as I walked through the door sobbing. I was embraced by my family and comforted before we sat down and tried to get our thoughts around what was happening. We escaped for the weekend to enjoy a beautiful family bushwalk. With every step, I marveled at how I could be so fit and well and yet have cancer that had already spread to my lymph nodes. Knowing things medically and experiencing things personally are two vastly different perspectives.
The biopsies confirmed grade 3 invasive breast carcinoma with spread to the axillary lymph nodes. I was unprepared for the week that followed, with further staging investigations and visits to a breast surgeon and an oncologist. I went to work in a daze and told them I would be needing some time off. By the end of that week, I was booked to begin chemotherapy.
The tests further revealed triple negative breast cancer with a very high Ki-67 (proliferation index > 80%). Suddenly, it was not just about dealing with breast cancer but desperately hoping it had not spread beyond my lymph nodes. Survival statistics of metastatic triple negative disease made for terrifying reading.
The moment I learnt there was no distant spread was a moment of sheer relief and joy. It was so strange to feel thankful for only local spread to lymph nodes, yet this is the perspective that life-threatening cancer brings.
I was due to start chemotherapy in 2 weeks, but this would be a few days before Christmas. I made the first of many active choices that felt right for me and gave me a sense of some control. I asked if we could wait a week. I needed time to process and prepare.
It was a great decision. I spent a superb Christmas with my family, feeling well. We ate, laughed and cried; our lives forever changed.
It is safe to say we were unprepared for the immediate onslaught of dose-dense doxorubicin and cyclophosphamide chemotherapy, but at least I felt ready to start rather than feeling stunned and scared. I feel this made an enormous difference to my perspective and how I managed with all the chemotherapy side effects.
I approached chemotherapy as I imagine many high performing, task-oriented doctors would. I learnt how to manage all the side effects and did everything I could to survive. I meditated daily and during chemotherapy. I managed 16 cycles of chemotherapy without a port and no major complications. I walked in nature every day except for the 72 hours after the chemotherapy infusions, when I needed rest and ice packs to hands and feet to minimise the risk of hand-foot syndrome. I even managed a run after the first few doses knowing the benefits of vigorous exercise. My hair fell out after the second round and I embraced my bald head.

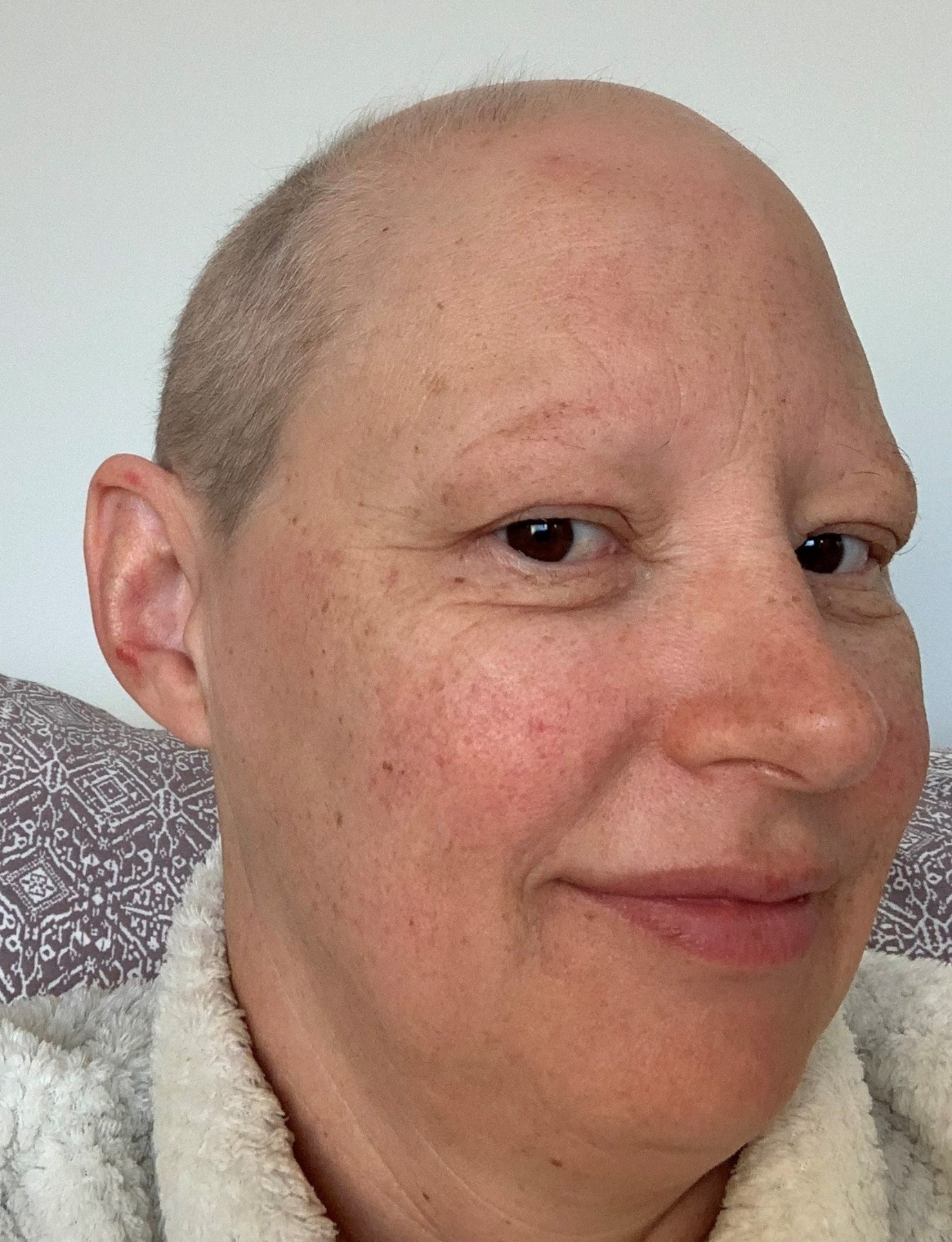
The twelve doses of paclitaxsol were better tolerated than the doxorubicin and cyclophosphamide, but each week came around so fast with no time to recover in between. Deconditioning despite daily exercise occurred rapidly. Combined with instant chemotherapy-induced menopause, mouth ulcers, constipation from antiemetics, sensitive skin, poor sleep from dexamethasone, and intense fatigue, it was a lot to manage. Just as I got some grey hair growth back on my scalp, I had lost all my body hair and my eyebrows and eyelashes fell out.

I had seen many patients through this journey. My medical knowledge and experience did not prepare me. I now know what they were not telling me. I had so much to learn! I also realise symptoms fade into the background when you are trying to survive.
After 5 months of chemotherapy, I tried to get some fitness back before surgery. The assistance of an exercise physiologist and cancer rehabilitation physiotherapist were invaluable, and I would like to see all cancer patients able to access them.
I was fortunate to have an amazing team and 5 months of chemotherapy to decide what treatment I wanted and plan for it. A month after finishing chemotherapy, I had a mastectomy, complete axillary lymph node dissection, and immediate autologous DIEP (deep inferior epigastric perforators) breast reconstruction.
Immediate autologous reconstruction meant I woke from the operation still feeling like I had a breast. Immediate breast reconstruction rates are low in Australia and more women requiring mastectomy for breast cancer should have access to this as an option. Access to the decision-making tool for breast reconstruction, BRECONDA, was valuable.
When you are busy saving your life, it is easy to believe losing a breast does not matter. However, the daily reminder of mastectomy can have more of an effect than just physical scars. Recovery has been slow and ongoing complications are part of my life now, yet the moment I learnt I achieved pathological complete remission was bliss. It was the miraculous news we had given our all to achieve.
As I return to work, I wish to use my experience to help others. The perspective of the patient journey I have gained will forever change me as a doctor. Being a patient has taught me so much more than my medical training could prepare me for. Strength, hope, determination, patience, courage and humour have been required. Understanding the fear, shame, guilt and embarrassment that accompanies the experience of doctors who become cancer patients is also important.
This patient perspective, through the lens of a doctor as the patient, will hopefully provide insights and reflection for all health professionals.
Dr Emma Warnecke is an Associate Professor in the Tasmanian School of Medicine at the University of Tasmania.

The statements or opinions expressed in this article reflect the views of the authors and do not represent the official policy of the AMA, the MJA or InSight+ unless so stated.
Loading comments…
Newsletters
Subscribe to the InSight+ newsletter
Immediate and free access to the latest articles
No spam, you can unsubscribe anytime you want.
By providing your information, you agree to our Access Terms and our Privacy Policy. This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.








