We need better ways of integrating robotic surgery into the training of junior surgeons, and this must start in Australian public hospitals, writes Professor Anthony Costello.
In July 2023, a remarkable conference occurred in Melbourne. The Society of Robotic Surgery held its annual meeting, attracting 1400 international and local surgeons, all robotic surgery enthusiasts. These surgeons represented the rapid adaptors or risk takers, mainly pioneers in their field. Clearly, there are many more than 1400 surgeons around the world, and most of them still use traditional laparoscopy and open surgery methods for almost all operations. Robotics is used in about 15.1% of surgeries where robots are available (here). But I suspect things are about to change and in a hurry.
Why was this conference remarkable? For the first time ever there were alternatives to the da Vinci system, first manufactured and sold by Intuitive Surgical California in 2000. This was a true changing of the guard moment as, until this year, Intuitive has been the sole provider of medical robot technology.
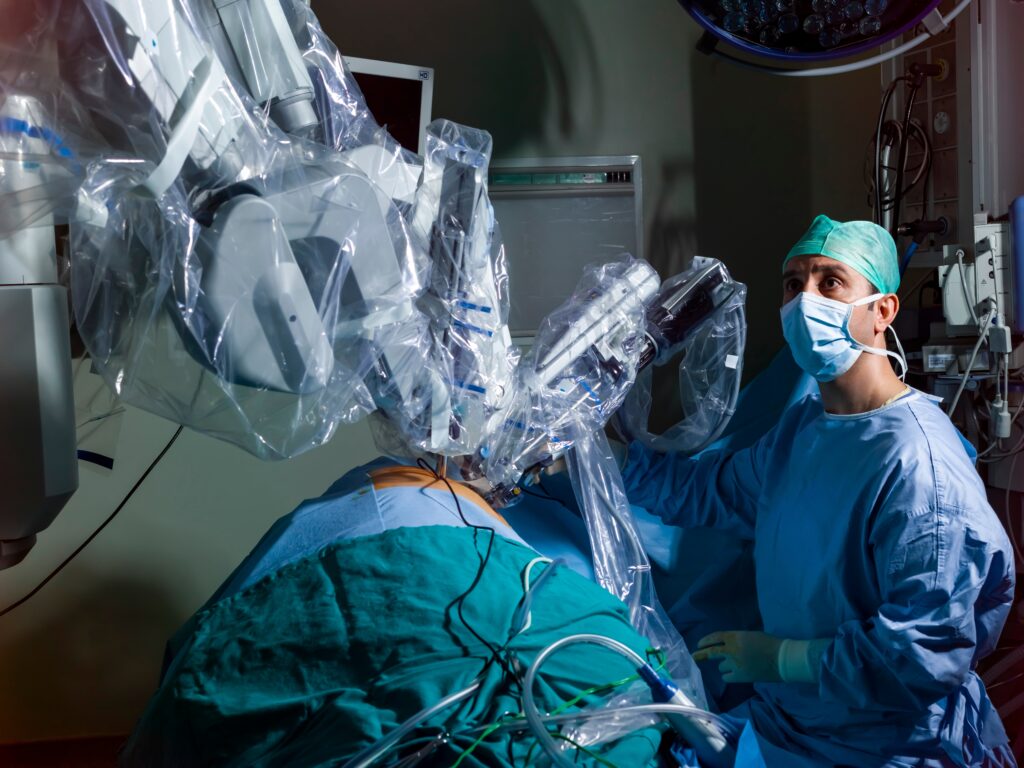
At the recent conference, ten new companies from countries including India, Korea, Japan, China, the United States, Italy, Greece and Germany presented innovative new robotic platform technologies for use in ear, nose and throat, cardiothoracic, abdominal pelvic and gynaecologic surgeries. I found out that most lung cancer surgeries in the US are now performed robotically, a figure backed up by a recent study (here). Competition in the market will significantly reduce cost of previously very expensive machines, facilitating the transition to robotic surgery in health care systems previously unable to afford the technology.
I witnessed a video performance of a coronary bypass grafting performed by an Indian cardiac surgeon who had designed his own robot. He demonstrated a device where a coronary artery graft was attached to a beating heart vessel and the coronary bypass graft was beautifully, miraculously robotically performed in four seconds. For me it was a Damascene moment; cardiac surgery may now undergo a renaissance, surgery could again compete with cardiology, a specialty where stent placement has overtaken or, in some cases, replaced cardiac bypass surgery for coronary artery disease.
New robots can be deployed endoscopically in the bronchus, stomach and colon to perform in endoluminal surgery (here). It is possible gastric bypass surgery could be an endoluminal procedure with stapling performed inside the stomach.
Robotic surgery began in the US in the year 2000 (here) and in Australia in 2003 (here). Why has adoption of such a marvellous technology that gives the surgeon vision 12 times magnification (here) in three dimensions with wristed instrument motion, scaled for tremor and filtered to remove jerky hand movements take so long to be embraced?
Engineers involved in the design and manufacture of surgical robots are well ahead of the ability of surgeons to harness the technology. The first surgeries performed in the early 2000s were only urologic, with other disciplines such as and gynaecology and general surgery coming later (here). There was a lot of opposition to the introduction of robots, mainly around high capital cost, fanciful marketing, and unsubstantiated claims by surgeons of extraordinary complication-free outcomes (here). One group even claimed 97% post-operative potency following radical prostatectomy in a cohort of men aged over 60 years, when potency rates in that age group are around 60% even in the most energetic cohort of men (here). In other words, surgery was making them more potent. Vigorous debate took place whether robotics was better than conventional laparoscopic and open surgery, and terms such as “gizmo idolatry” were bandied about (here and here).
After three years using a da Vinci robot to perform radical prostatectomy, I was totally convinced the future in surgery would be completely robotic.
Arguments against change in technology were everywhere but I believed the robot train left the station around 2007. We were able to perform radical prostatectomy robotically as day case, an operation which previously done open kept the patient in hospital for seven days, with a 1400 mL average blood loss (here).
The robot is a very powerful computer interface between the surgeon and patient able to provide real time three-dimensional wristed hand movement with seven degrees of freedom in an ergonomically excellent surgical position for the surgeon. Widespread deployment was hampered mainly by high capital machine and instrument cost (here). Robots in Australia were only available in the private sector, the public sector unable till now to provide the capital cost of these machines.
In Australia, we are now faced with two major public health issues: first, equity and access; and second, robotic surgery training. Many public patients are denied access to the best technology for their condition because of the absence of robot machines in their public hospitals — only some public hospitals have them (here, here and here).
Surgical trainees work only in the public sector where there are no robots. At the present, surgeons in Australia take seven years to train but may never see a robot. When they go into practice in the private sector, the robot will be the technology that most of them will be using. A recent study found a similar situation in the United Kingdom.
There are many barriers to introduction of robots into our health system (here). The methodology or curriculum upon which surgical training is based is the residency program published by William Halsted, a Johns Hopkins surgeon, in 1904 (here). This brutal system was not for the faint hearted. Training was restricted to single men who lived in a residence for seven years. There were no holidays and few weekends not on call. Our present system based on this pedagogy is not particularly different 120 years later. It is no longer fit for purpose. Our surgery trainees are an exploited workforce doing many unrostered, unpaid overtime hours with mostly unsatisfactory training in the past century’s operative techniques (here).
In my view, we need to change our surgical training methodology. Robotic surgical training lends itself to be modularised, using algorithms and objective measures for assessment of proficiency. The seven-year training program is too long and could be shorter and with better robotic surgical training. Improved surgical education should reduce surgical complications.
Many surgical colleges, here and overseas, are now exploring ways to teach surgical robotics (here, here and here). Education is hampered by the absence of surgical trainers with the expertise in robotics who are themselves comfortable teaching a junior surgeon. A concept of shadow learning has been postulated by Mathew Beane, where the robotics training surgeon is not comfortable to hand over the controls to a trainee because they are still learning how to use a robot themselves. Thus, the trainee shadow learns by observation not by operating on the patient (here).
In 2023, surgeons still train on cadavers and live animals, which presents ethical and financial problems. These simulations are single training events. The airlines have shown us that simulation training can replace in-cockpit training and that, by the time a pilot has completed hours of simulation, they are ready to fly the aeroplane. With simulation training, airlines have reduced their accident rate to minuscule, but we still have a 30-day 17% readmission rate after major surgery due to complications. In 2022, relatively inexpensive high fidelity synthetic human organ models became available to replace cadavers and live animals. This new method developed in Melbourne allows multiple operative simulation experience to achieve surgical proficiency before actual mentored human surgery (here).
With the cost reduction of the robot, surgeries such as appendicectomy, cholecystectomy and hernia repair may soon all be done using a robot. There will likely be a robot in every operating room and a robot for every surgical specialty. Robots remove tremor and allow more accurate surgery, great for microsurgeons and their patients.
We live in exciting times for Australian hospitals and surgeons who wish to embrace robotic technology.
Professor Anthony Costello is an Honorary Professor at the Department of Surgery at the University of Melbourne and is a surgeon at Royal Melbourne Hospital.
The statements or opinions expressed in this article reflect the views of the authors and do not necessarily represent the official policy of the AMA, the MJA or InSight+ unless so stated.
Subscribe to the free InSight+ weekly newsletter here. It is available to all readers, not just registered medical practitioners.
If you would like to submit an article for consideration, send a Word version to mjainsight-editor@ampco.com.au.

 more_vert
more_vert
There are no randomised controlled trials demonstrating any superiority of robotic surgery with any operation. The only definite thing is it is much more expensive. Let’s do the trials to demonstrate a potential benefit before embracing this technology. At the moment it is just a marketing tool that makes an average or below average surgeon look good.
We saw a similar revolution when laparoscopic surgery developed in the 1990s, now routine in operating theatres for many ( not all ) abdominal surgeries. Operating times have reduced dramatically and recovery is quicker than with open procedures. .However the fundamental surgical techniques are essentially similar to open laparotomies, with some innovations and adaptations. At the start, the adoption of laparoscopic techniques proceeded too quickly and sometimes inappropriately and there is no doubt many patients suffered, before surgical common sense prevailed and it found its correct level with the recognition that some abdominal procedures, especially in the emergency situation still are best and most safely done by traditional laparotomy. The problems I see with robotic surgery are that it requires a totally different approach, a new paradigm, and there will be exceptionally long learning curves for surgeons in mid career not brought up with the technology. Most significant are the costs and logistics of providing the equipment and training outside of major city hospitals. Dr Costello’s enthusiasm is admirable but needs to be tempered with realism and the limitations on availability of highly expensive and complex machinery and the learning curves required. Many surgeons doing small numbers of cases each is not the answer. Small groups in each appropriate specialty need to develop expertise in an unhurried fashion to a point where they can properly teach others. The old saw ” see one, do one, teach one ” is highly inappropriate. At the moment surgeons are lining up to use the robot mainly through a fear of being left behind, and i see real parallels with the excesses of the early days of laparoscopic procedures. It is also vital that in the adoption of exciting new technologies we do not forget fundamental surgical principles surgical lessons learned by our surgical forebears through long and often bitter experience.
Simple solution. Found the Australian College of Robotic Surgery. Get some machines donated for your teaching hospitals (Da Vinci or whoever will see the business case) and run your trainees in competition to the RACS (I’m sure the ACCC would admire that initiative).
Trainees could either be fresh out of medical school (younger, more adept at psychomotor learning) or could be RACS Fellows as a post-fellowship extension. If you feel really brave, offer a university Bachelor of Robotic Surgery degree to high school leavers, where like vets and dentists, they graduate as fully-licensed practitioners. Eliminate the bloatware of medical schools (you don’t need to understand leukaemia, schizophrenia, or neurophysiology to be an abdominal surgeon) to make a surgical degree, and your early 20s graduates are ready to staff the public hospitals.
Of course, it remains a very temporary stopgap. Once Da Vinci and Chat GPT version 25 get together, the human surgeon will be redundant. Just ask your Lasik machine.
I fully support your opinion. I have seen robots doing wonders in the operating theatre with less operating time, less trauma to patients and quicker revovery time. It is a win-win for all. Therefore, the Medical profession and the government need to cooperate to speep up the new training process for junior surgeons.
Brilliant insights on robotics,
Next 5 years will revolutionise and many
patients will be pleased with their outcome.