EXPERTS say better support for GPs is vital to increase screening for obesity, after an Australian study revealed that quantitative measures of patient obesity identified in national guidelines are being recorded at suboptimal rates.
Professor Mark Harris, director of the Centre for Obesity Management, Prevention and Research Excellence in Primary Health Care at the University of NSW, told MJA InSight the low documentation in general practice of a patient’s body mass index (BMI) and waist circumference had potential implications for the quality of care.
“By not recording this data, we’re missing an opportunity to identify and manage a patient’s risk for diabetes and cardiovascular disease early on.”
Professor Harris coauthored the study, published this week by the MJA, which assessed the documentation of measures recommended in NHMRC clinical guidelines for managing overweight and obesity. (1)
The retrospective analysis of 270 426 adults used patient data between 2011 and 2013 from a general practice database in Melbourne, specifically examining the first two recommendations of the NHMRC guidelines relating to the documentation of BMI and waist circumference. (2)
They found 22.2% of the patients had a BMI and 4.3% a waist circumference recorded in their computerised medical records. There were variations in BMI documentation across age and sex, with those aged over 75 years more likely and women less likely to have a documented BMI.
Patients with diabetes who were prescribed diabetes-related medication and patients with hypertension or hyperlipidaemia were also more likely to have a documented BMI.
The researchers said their results highlighted the need for improved support for GPs to increase levels of obesity screening in accordance with NHMRC guidelines. This included implementing programs to enhance the organisational capacity of general practices, and to facilitate the standardised collection and recording of data.
They also called for further research to assess how the documentation of obesity-related clinical information changes over time, and to examine the barriers and enablers to increased obesity screening.
In a written statement to MJA InSight, the president of the Royal Australian College of General Practitioners (RACGP) Dr Frank Jones said the study indicated that GPs could be doing better when it came to screening for obesity.
“There are higher rates of GPs screening for smoking and ideally obesity screening should reach the same rate of recording”, Dr Jones said.
He identified the time pressures faced by GPs as the main factor behind the lower screening levels for obesity and suggested that “for some practices, using practice nurses to record a patient’s BMI and waist circumference may be a more efficient use of time”.
He said the RACGP recognised the important role GPs played in helping people make lifestyle changes and offered a range of resources to support doctors, including the recently updated SNAP guidelines — Smoking, nutrition, alcohol, physical activity (SNAP): a population health guide to behavioural risk factors in general practice. (3)
Professor Harris told MJA InSight that while measurement documentation was not a matter of life and death for a patient, it was a valuable tool to ensure diagnoses were accurate, because “abdominal obesity is underestimated and can be difficult for GPs to identify, particularly in taller people, by just looking at a patient”.
Dr Cilla Haywood, a physician at Austin Hospital Weight Control Clinic and consultant in geriatric medicine, general medicine and obesity management at Northern Health, Melbourne, agreed, but said it was important to consider patient measurements as just one component of obesity management.
Just because some GPs were not making an official record of BMI and waist circumference did not mean the issue of obesity wasn’t being sufficiently recognised, Dr Haywood told MJA InSight.
“Usually if there is an issue with weight, both the GP and patient are aware of it, whether or not there have been formal measurements recorded.”
However, Dr Haywood said the MJA study did demonstrate that the management of obesity was a rapidly evolving field, and highlighted the importance of keeping GPs up to speed on the latest clinical research.
“Measurement of BMI is a first step to managing obesity, but there are many steps after, and GPs need to be supported throughout each stage.”
1. MJA 2015; Online 13 April
2. NHMRC. Clinical practice guidelines for the management of overweight and obesity in adults, adolescents and children
3. RACGP 2015; SNAP
(Photo: sunabesyou / shutterstock)

 more_vert
more_vert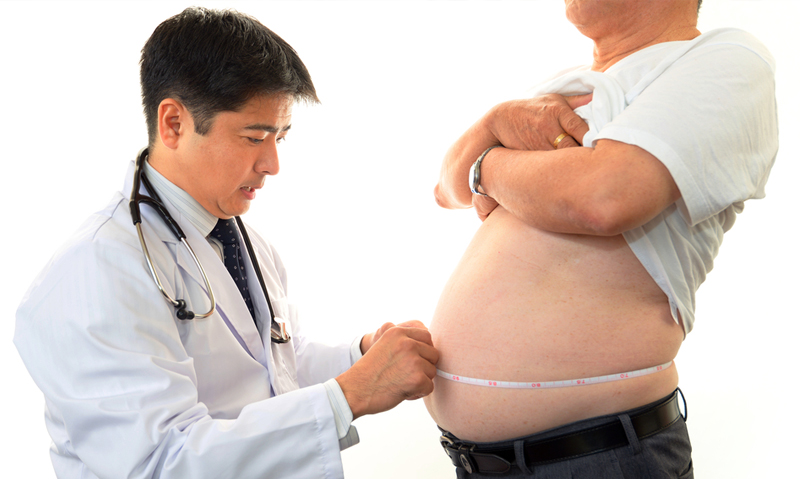
I think there are three main reasons to measure and record BMI and WC
1. Guideline recommendations for management are tailored to risk (defined by BMI and WC category) based on evidence (see NHMRC Guidelines)
2. As the first of the the 5As (Assess) it is valuable first step in explaining the risk associated with obesity to the patient and this has been shown to increase patient motivation to change (2 studies)
3. It is important at a practice level to audit risk in the practice population and determine if treatment is appropriately tailored to risk.
Of course it needs to be followed by the other “A’s” – advice, agree (goal setting), assist (referral), arrange (follow up). It is also important not to stigmatise obese patients.
I generally do measure BMIs and waist circumference, but how strong is the evidence that doing so makes a difference to patient outcomes, particularly if the patient isn’t motivated to make lifestyle changes? Occasional patients refuse to be weighed, and all of these would fall into the obese or morbidly obese category. As Dr Haywood points out, this doesn’t mean the patient and I aren’t aware of the issue, and it certainly doesn’t result in less aggressive screening for cardiovascular risk factors in such patients.
This problem can be solved by using the Doctors’ Control Panel software (http://www.doctorscontrolpanel.com.au) that reminds the doctor or nurse via an on screen display, and that also has versions that print a reminder about this for the patient when they arrive for a consultation.
In my day the only scales I trusted were the ancient canti-lever ones, as did the patients/clients.The old spring-loaded floor scales were common but next to useless. How trustworthy are modern floor scales?