Developments in hyperacute stroke management for patients with renal disease are encouraging, but they also underscore the importance of ongoing vigilance and adaptation in the provision of stroke care.
In the fast-paced world of hyperacute stroke management, it is often mentioned that “time is brain”. Every minute saved can mean the difference between life and death or permanent disability for stroke patients.
Traditionally, administering contrast agents during hyperacute stroke management raised fears of contrast-induced nephropathy, especially in patients with chronic kidney disease. This apprehension often translated into delaying essential imaging scans, potentially compromising patient outcomes. Nevertheless, recently updated guidelines and studies have lessened these fears, highlighting that chronic kidney disease or haemodialysis are not absolute contraindications to receiving iodinated contrast (here).
It is imperative to re-evaluate our practices to align with current evidence-based guidelines. Recent studies have also indicated that the use of additional contrast medium to facilitate imaging techniques, such as computed tomography perfusion, does not increase the risk of acute kidney injury. These findings have prompted revisions in departmental protocols, emphasising the importance of timely imaging for hyperacute stroke management.
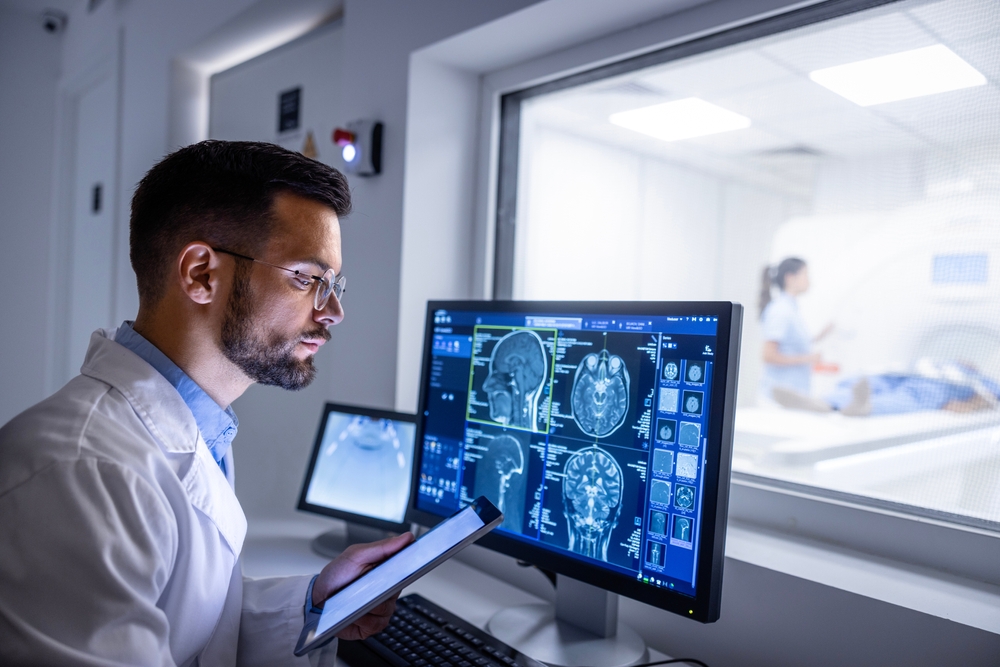
But how do these shifts in practice potentially affect actual delivery of care? To answer this question, a comprehensive study was conducted over a five-year period (2017–2021) across multiple stroke units in South Australia. The aim was to assess the association between pre-existing renal disease and the timeliness of hyperacute stroke care, focusing on key metrics such as symptom-onset-to-door time, door-to-scan time, door-to-needle time, and door-to-groin-puncture time.
The results of this study, encompassing 2960 patients, provided insightful revelations. Contrary to historical concerns, there were no significant delays observed in hyperacute stroke management for patients with renal disease (Table). This finding underscores a paradigm shift in stroke care, where renal impairment no longer serves as a barrier to timely interventions.
| Time parameter | Patients not fulfilling criteria for pre-existing renal disease (n=2879) Time interval (minutes) | Patients with pre-existing renal disease by selected criteria (n=81) Time interval (minutes) | P value |
| Symptom-onset-to-door time median (IQR) | 98.0 (65.0–203.0) | 92.0 (69.0–138.0) | 0.24 |
| Door-to-scan time median (IQR) | 27.0 (19.0–42.0) | 27.0 (22.0–39.0) | 0.6 |
| Door-to-needle time median (IQR) | 65.0 (51.0–83.0) | 63.0 (55.0–88.0) | 0.74 |
| Door-to-groin-puncture time median (IQR) | 103.0 (82.0–126.0) | 99.0 (96.0–122.0) | 0.65 |
Delving deeper into the data, it’s probable that protocols for acute code stroke management play a pivotal role in ensuring equitable and efficient care delivery. These protocols, tailored to accommodate the latest evidence and guidelines, have likely mitigated any potential delays associated with renal disease. By standardising procedures and streamlining workflows, stroke units have optimised their capacity to deliver timely care to all patients, regardless of comorbidities.
Although this study’s findings are encouraging, they also underscore the importance of ongoing vigilance and adaptation in the provision of stroke care. As the evidence regarding hyperacute stroke management continues to evolve and treatment modalities advance, it’s imperative for health care systems to remain agile and responsive. By embracing evidence-based practices and leveraging innovative technologies, stroke units can further enhance their ability to deliver timely, appropriate and effective care to all patients, irrespective of their comorbidities.
In conclusion, this study did not find a difference in hyperacute stroke management for patients with renal disease, compared to those without. Moving forward, health care providers must continue to collaborate, innovate and adapt to ensure that every stroke patient receives timely and comprehensive care.
Dr Rudy Goh is a neurologist with research interest in stroke and interventional neuroradiology.
Dr Stephen Bacchi, MBBS, PhD is a neurology registrar with interests in clinical research and teaching. Stephen’s PhD focused on clinical applications of artificial intelligence in stroke and general medicine.
Additional authors: Joshua G. Kovoor, Aashray K. Gupta, Christopher D. Ovenden, Minh-Son To, Andrew Moey, David Schultz, Jordan Li, Timothy Kleinig, Jim Jannes.
The statements or opinions expressed in this article reflect the views of the authors and do not necessarily represent the official policy of the AMA, the MJA or InSight+ unless so stated.
Subscribe to the free InSight+ weekly newsletter here. It is available to all readers, not just registered medical practitioners.
If you would like to submit an article for consideration, send a Word version to mjainsight-editor@ampco.com.au.

 more_vert
more_vert