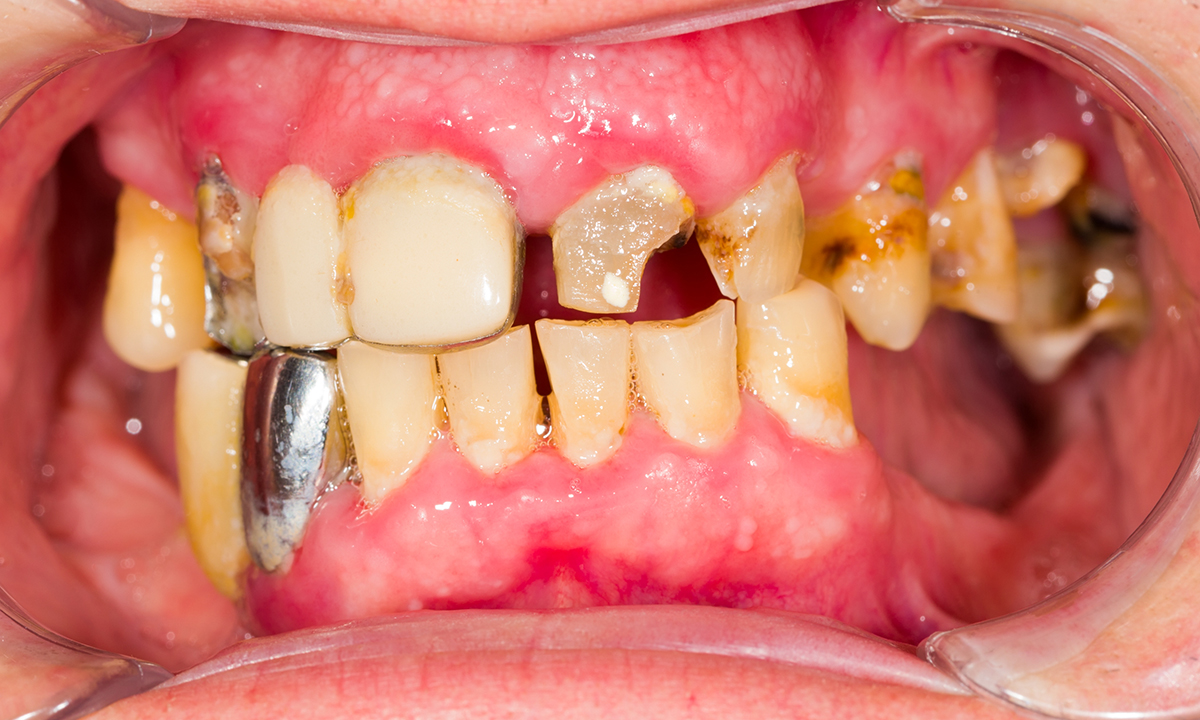
THREE in four frail elderly patients in acute care present with poor oral health and, in most cases, this fails to improve over a 1-week hospital stay, Australian researchers have reported.
In a study published in Age and Ageing, the oral health of 575 patients admitted to acute geriatric care at two NSW hospitals was assessed. The researchers found that 76% of patients had oral cleanliness scores in the “not healthy” range, with food particles, tartar or plaque evident in their mouth, teeth or dentures.
After 7 days, 206 patients were reassessed and 72% (149) were in the “not healthy” range. Of the 206 patients, 62% (127) had the same oral health score as on admission.
Lead author Jennifer Gibney, a clinical researcher with Concord Hospital’s Centre for Education and Research on Ageing, said that there were several reasons why this group of patients may present with poor oral health.
“It may be because of poor oral health at home. They may not be able to get to a dentist because they rely on other people to drive them. There is also the cost of going to a dentist, or they may have comorbidities, such as osteoarthritis, that make it hard to brush their teeth,” Ms Gibney told MJA InSight.
Also, she said that patients admitted into geriatric care often had reduced alertness, or may be confused or delirious.
“They have behaviours that may impact people’s ability to help them with their oral hygiene,” Ms Gibney said, who is also a speech pathologist.
A lack of standard oral health procedures in many hospitals, she said, meant that poor oral hygiene was often not dealt with after hospital admission.
In a 2015 study conducted by Ms Gibney, hospital nursing staff reported several barriers to supporting oral health care, including patient behaviours, lack of resources and patients’ physical difficulties.
Consultant geriatrician Associate Professor Vasi Naganathan emphasised that this latest study was conducted among frail elderly patients with multiple comorbidities.
“There’s a high proportion of people who have poor oral health, and for some people it gets worse in hospital. This is perhaps not surprising, considering how sick they are,” said Professor Naganathan, a co-author of the Age and Ageing study.
“These are people who maybe have two infections at once, they may be delirious, they may have pain, fractures.”
Professor Naganathan said that efforts to improve oral health could potentially reduce the rate of aspiration pneumonia, which affects a small proportion of patients admitted to geriatric care.
“But it’s a big ‘may’,” he said. “There is an argument that if you clean up people’s mouths, they may be at less risk of aspiration pneumonia and you may have more freedom in terms of what you can give them orally.
“But there is the counter argument: with so many other [health problems] to address, will fixing up their oral health make any difference in that context?”
These are questions that the research group is hoping to answer in the future, with one study already underway to evaluate the impact of having an oral health therapist on wards and supporting nurses to provide oral care to patients.
Further research would then be needed to assess the impact of these interventions on health outcomes, Professor Naganathan said, noting that such a study would be difficult.
Professor David Manton, chair of the Australian Dental Association’s Oral Health Committee, said that this latest research raised a broader problem of oral health among elderly people who were increasingly keeping their own teeth.
Professor Manton said that 25–30 years ago about 70% of 70-year-olds had full dentures, but that this had decreased to around half in patients in nursing homes, with probably an even smaller proportion in the general population.
“As each decade goes on, that will continue to decrease,” he said.
However, Professor Manton said that oral health care procedures in hospitals and nursing homes had not evolved to reflect this change in patients’ oral care needs.
“It used to be [that patients would] take their teeth out, give them a scrub, and put them back in or maybe leave them in the drawer by the bed – it’s really changed the concept of oral health in this population group,” he said.
“Now, when people end up in nursing homes [or in hospital], the nursing staff and associated staff are expected to look after the oral health of the patient, and most did not have training or the allocated time to do that.”
To find a doctor, or a job, to use GP Desktop and Doctors Health, book and track your CPD, and buy textbooks and guidelines, visit doctorportal.

 more_vert
more_vert