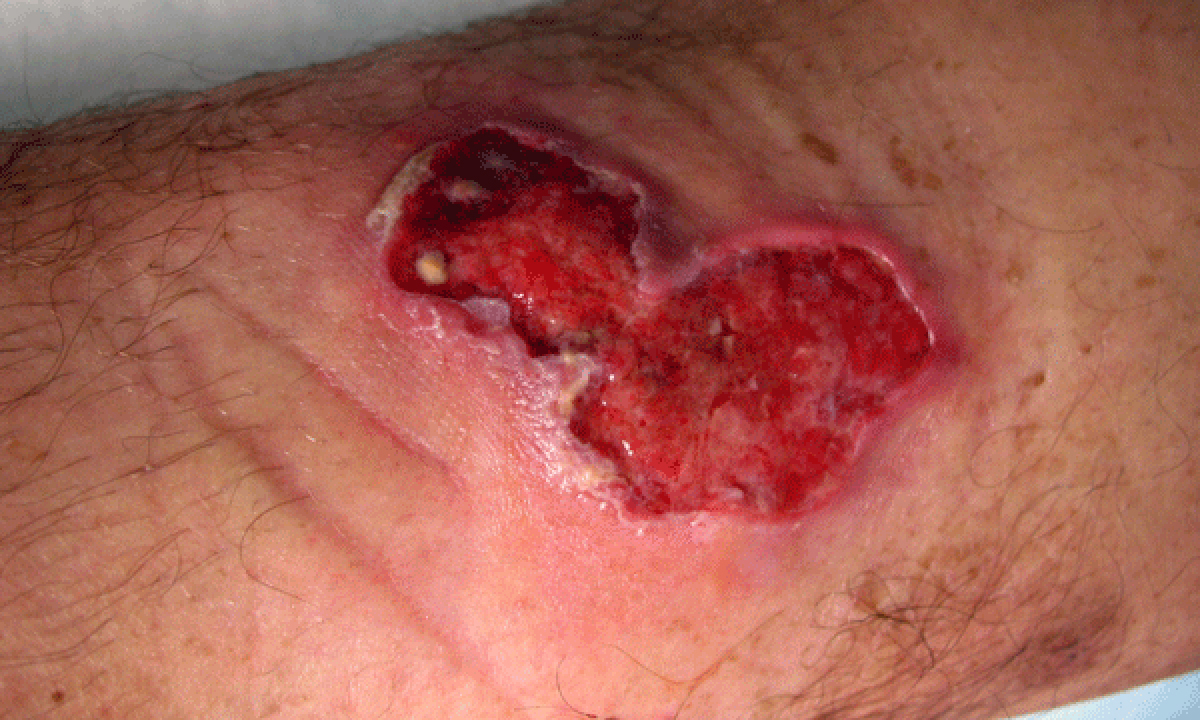
BURULI ulcer should be on the radar for GPs across Australia as cases of the geographically restricted Mycobacterium ulcerans infection continue to increase and spread from areas of Victoria where it is already endemic to Melbourne’s south-eastern bayside suburbs, says infectious diseases specialist Professor Paul Johnson.
Professor Johnson, who is Director of the World Health Organization Collaborating Centre for Mycobacterium ulcerans and an infectious diseases physician at Austin Health, said that any person who visited an endemic area – even for just a few hours – was at risk of the infection.
“GPs in Australia need to know about Buruli because people can visit an area like the Mornington Peninsula or the Bellarine Peninsula or far north Queensland on their holidays, and be there for as little as a few hours, then present 5 months or more later with a strange progressive skin lesion that no one in their area has ever seen before,” he told MJA InSight.
“You need to think of the diagnosis in order to order the right test to diagnose Buruli.”
The number of confirmed cases of Buruli infection began to increase steeply from 2000, with 162 cases confirmed in Australia for the calendar years 2013–2014, 152 of which were in Victorian endemic areas.
In 2015, there were 106 cases in Victoria, and this year so far 59 cases have been recorded.
Buruli ulcer – which is also called “Bairnsdale ulcer” in Victoria and “Daintree ulcer” in north Queensland – was first recognised as a new disease caused by a novel pathogen in Australia in the East Gippsland region of Victoria in the 1930s, but began to appear closer to Melbourne from the early 1990s.
The disease is endemic in towns on Victoria’s Mornington Peninsula and the Bellarine Peninsula, and is beginning to occur in the inner south-eastern bayside suburbs including Beaumaris, Hampton and Brighton.
Smaller numbers of Buruli infections have also occurred in Queensland, between Mossman with the Daintree River, and coastal southern Queensland near Yeppoon. But Professor Johnson said there was less indication of geographic spread from these areas.
Professor Johnson said that wider recognition of the changing high risk areas was key to enabling timely detection of the infection.
“If a patient has been to any of these areas, even once, they’re at risk, even though it’s a very small risk,” he said.
Professor Johnson said that residents and visitors to these areas could be advised to protect themselves from insect bites, and to clean and cover any cuts sustained outdoors.
He said that increasing populations in the affected coastal areas as well as the spread of the organism to new areas were partly driving the increase in cases.
“More people are living down in the various coastal areas of Victoria,” he said. “We also have evidence that the disease may occur in possums, so it could be that what we are looking at is an epidemic in possums, with humans as a spill-over host, and we think that the most common mode of transmission to humans is biting insects.”
However, he said that uncertainty remained about transmission and why the infection, which is also found in 33 other countries, was limited to certain geographical areas.
The early signs of Buruli can be quite non-specific, Professor Johnson said, with a painless nodule or plaque on the skin that slowly progresses, sometimes over weeks, to an ulcer.
Patients may recall an insect bite or scratch at the site, and rarely the infection is accompanied by fever or other symptoms. Once fully developed, Buruli causes a deeply undermined ulcer.
Some patients may also present without a nodule or ulcer, but a raised reddish plaque or swelling of a whole limb resembling bacterial cellulitis which does not respond to standard treatment.
Adding to the diagnostic challenges is the variable incubation period, which is a median of 4.5 months, but can range from 3 weeks up to 7–8 months.
“Early diagnosis leads to minimal damage, so it’s important to think of the diagnosis and do the right test,” he said. “The diagnostic test is very accurate.”
Professor Johnson said that a diagnosis could be made directly from an ulcer swab but it was essential to specify polymerase chain reaction (PCR), smear and culture for M. ulcerans and Buruli ulcer on the pathology request. Standard laboratory tests will not detect M. ulcerans.
If an ulcer has not yet formed, a biopsy may be needed but the diagnosis is also easy to confirm by PCR on fresh tissue.
“We evolved a way of using antibiotics to assist with surgery and that has now turned into using antibiotics alone in about half of cases, but it’s not to the exclusion of surgery,” he said. “When antibiotic treatment is finished, there may be a skin defect remaining so we may still need surgery to get the best outcome.”
Professor Johnson said that antibiotic treatment was initially thought to be ineffective because lesions would often worsen after being treated with antibiotics; however, this has now been recognised as an intense inflammatory response to dying bacteria.
Professor Johnson is scheduled to speak at an MJA infectious diseases seminar in Melbourne in September 2016. For more details visit doctorportal.
Latest news from doctorportal:
- Invest in health to avoid political disaster, Gannon tells Govt
- Doctors need to be taught how to discuss their patients’ excess weight
- New plan to find poor performing doctors
- Remote Australians more likely to be hospitalised with heart-related issues

 more_vert
more_vert